Lumbar spondylosis/ Targeted Conditions
What is degenerative lumbar spondylosis?
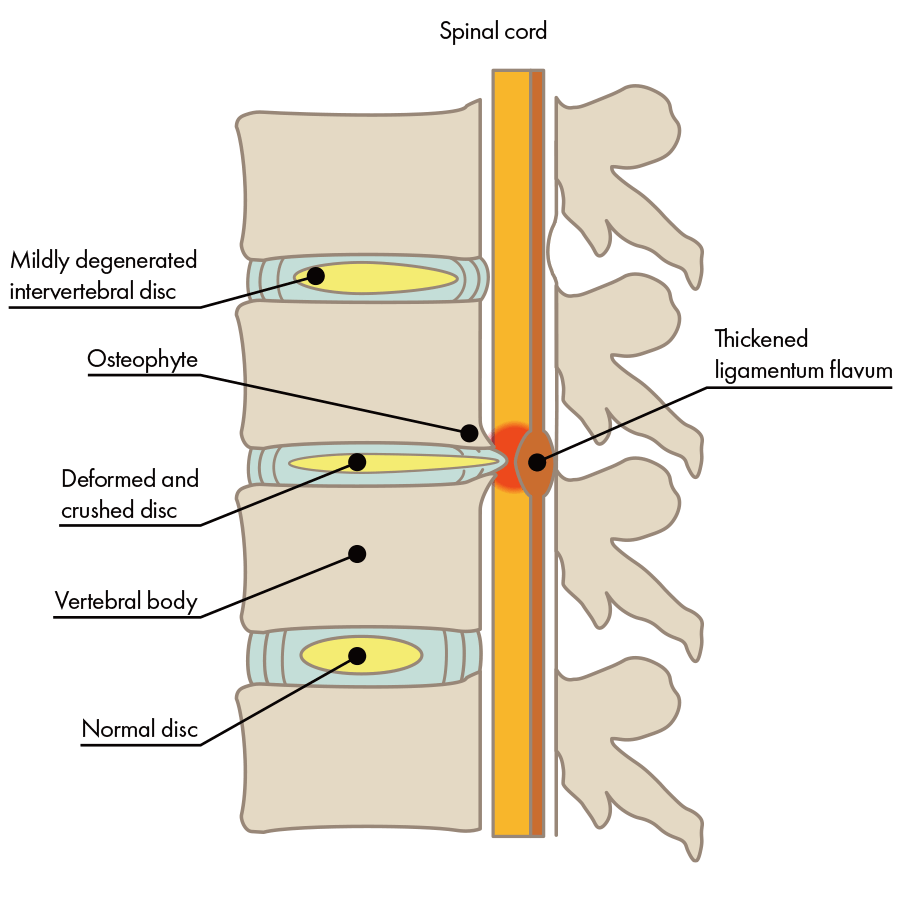
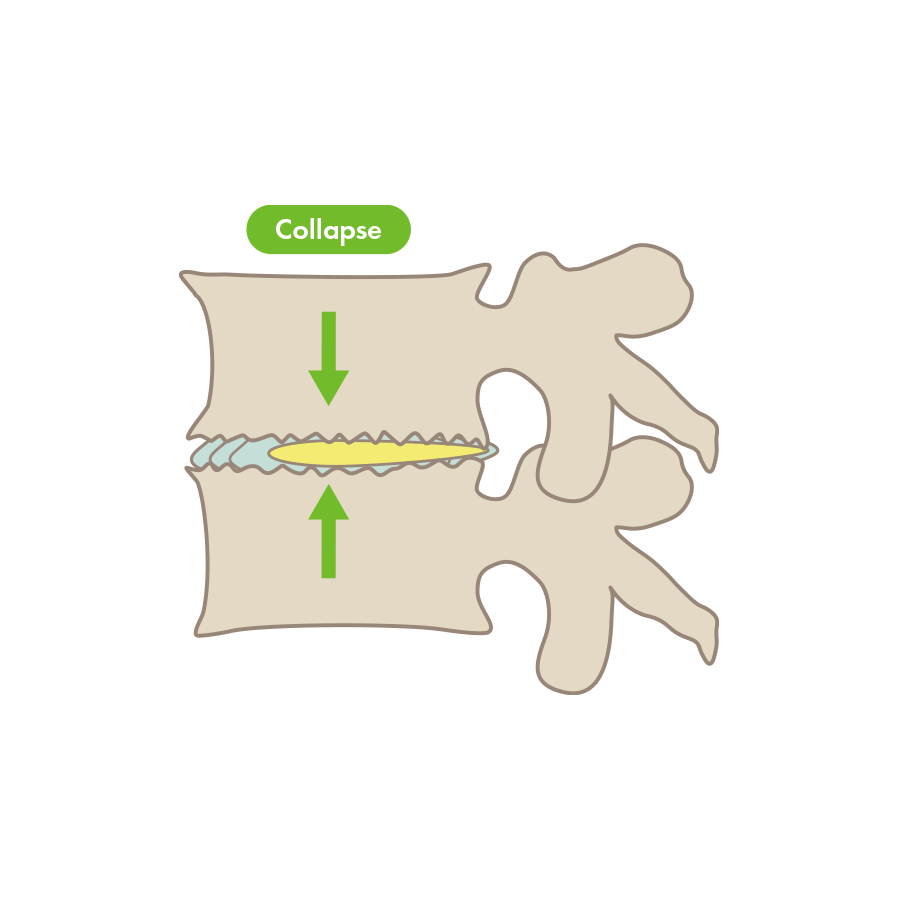
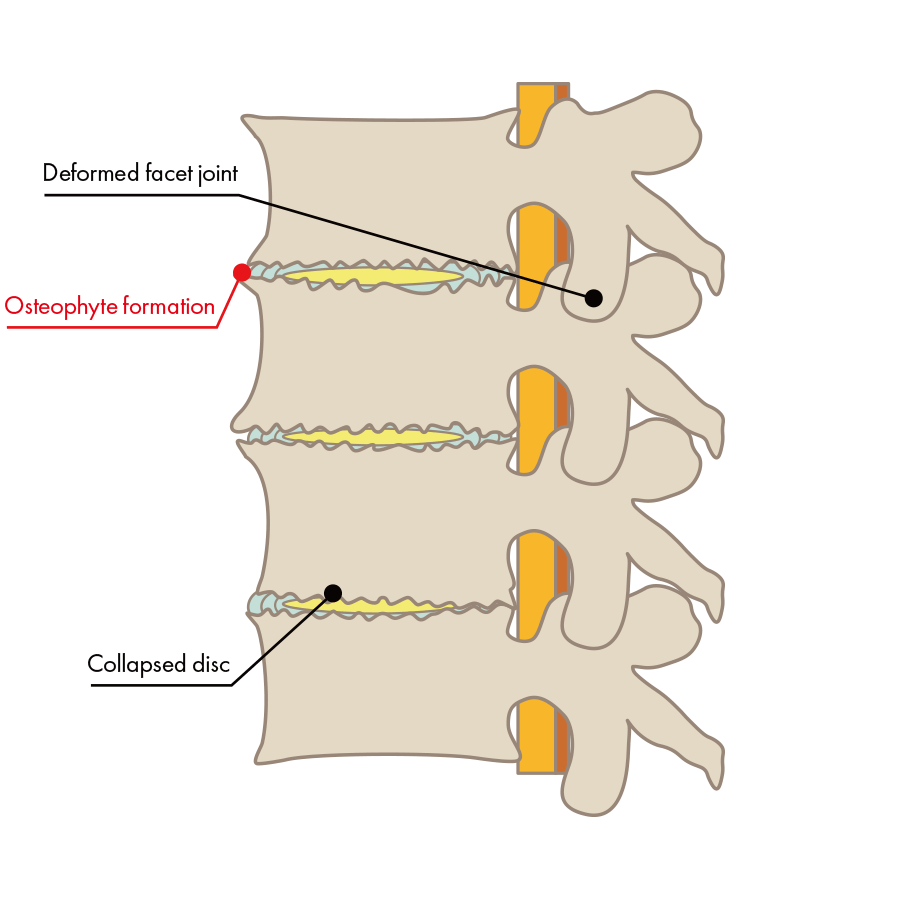
Degenerative lumbar spondylosis is an age-related alteration in the lumbar spine that can lead to the formation of bone spurs (also called osteophytes), or to back pain caused by a deformity of the spine. As the deformity progresses, it may transition to spinal stenosis and other conditions.
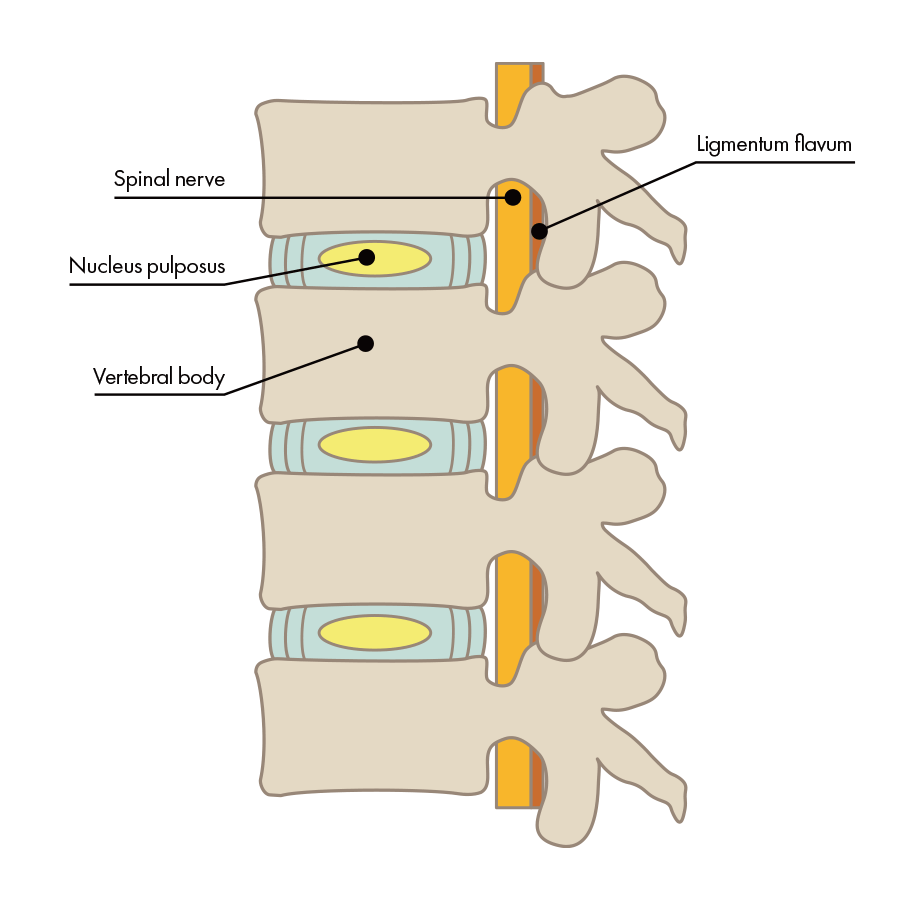
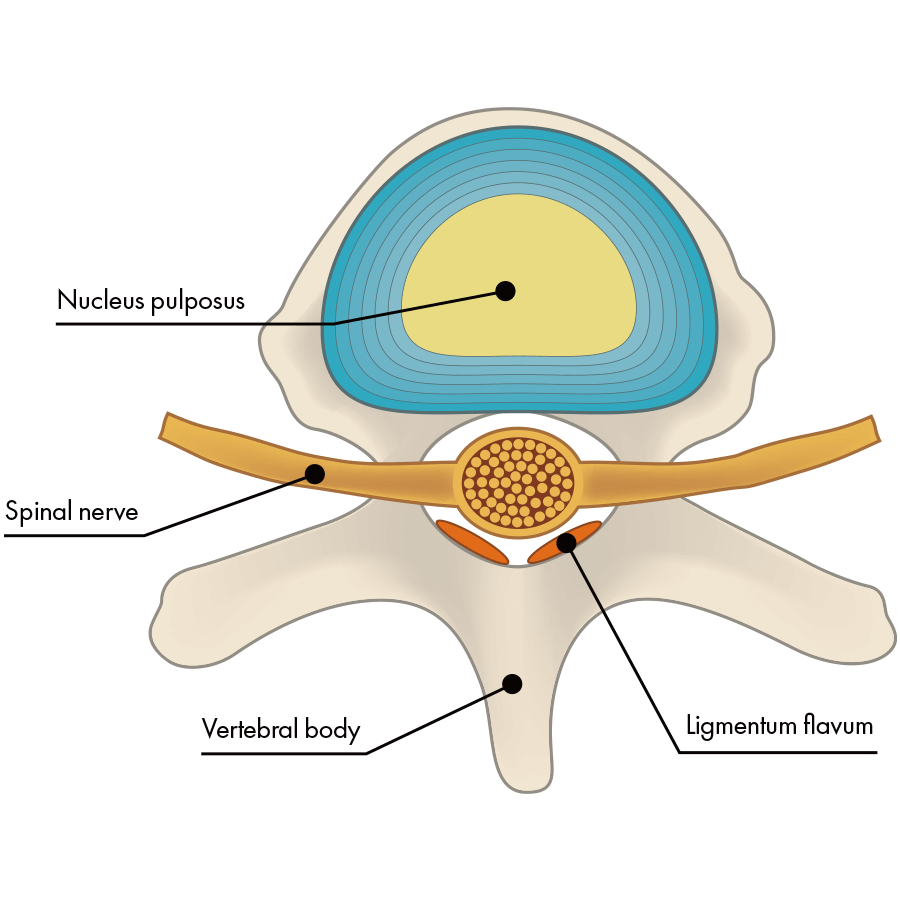
Normal intervertebral disc
Causes of degenerative lumbar spondylosis
Degenerative lumbar spondylosis is mainly caused by the effects of age, the work environment and physical exercise.
These factors may result in the following:
- Disc degeneration
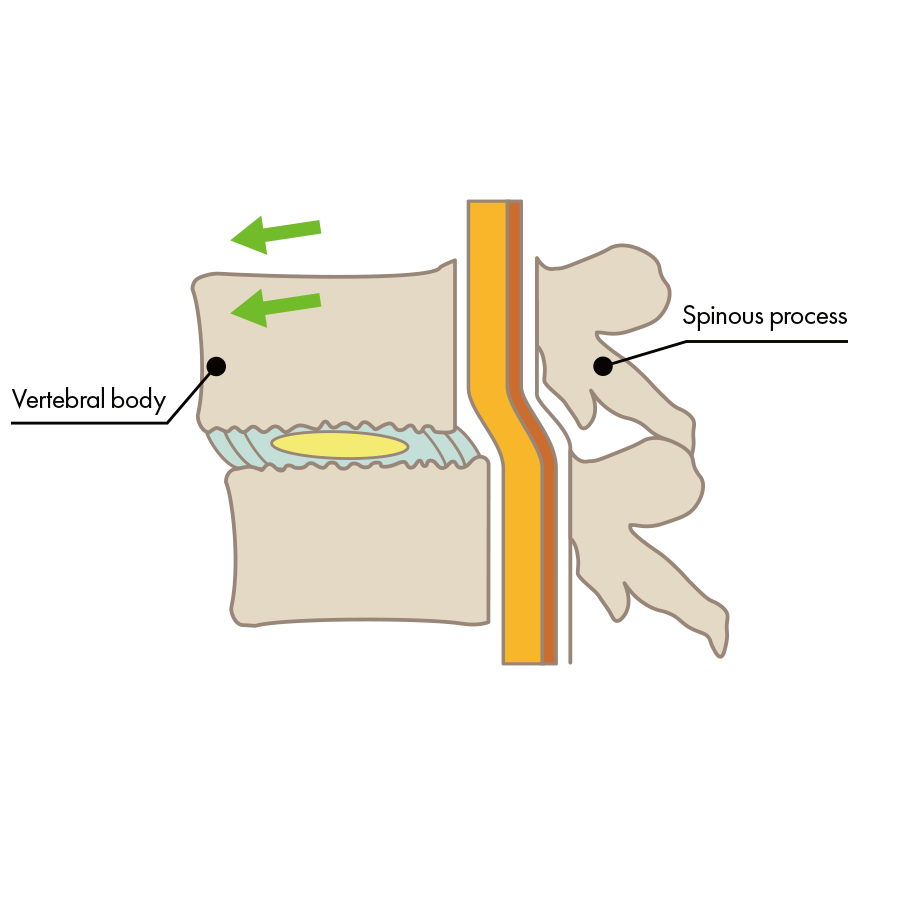
- Lumbar spine instability
- Bone deformity and formation of bone spurs due to repeated contact between the lumbar vertebrae
The progression of these deformities and degeneration may cause damage to bones, discs, and nerves, all causing inflammation, which in turn causes pain. Along with this degeneration and deformation, the degeneration also spreads to the surrounding joints and ligaments. As the deformity progresses, the narrowing of the spinal canal and nerve pathways may lead to spinal stenosis, spondylolisthesis, and scoliosis, among other conditions.
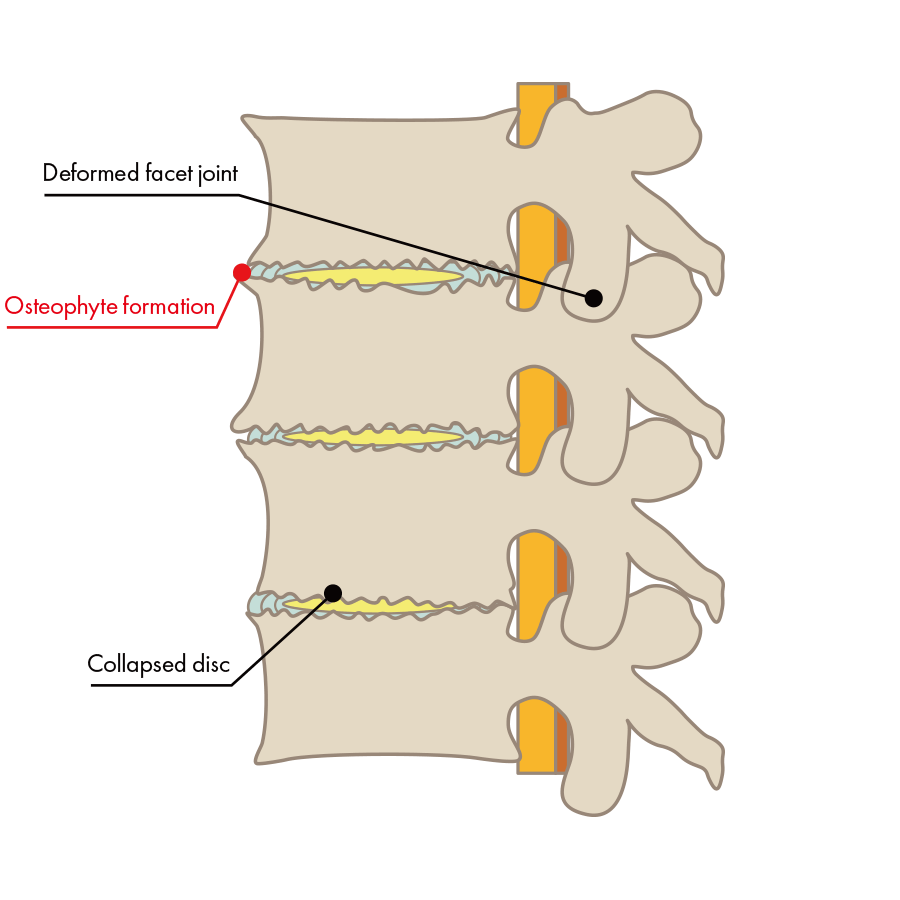
Symptoms of degenerative lumbar spondylosis
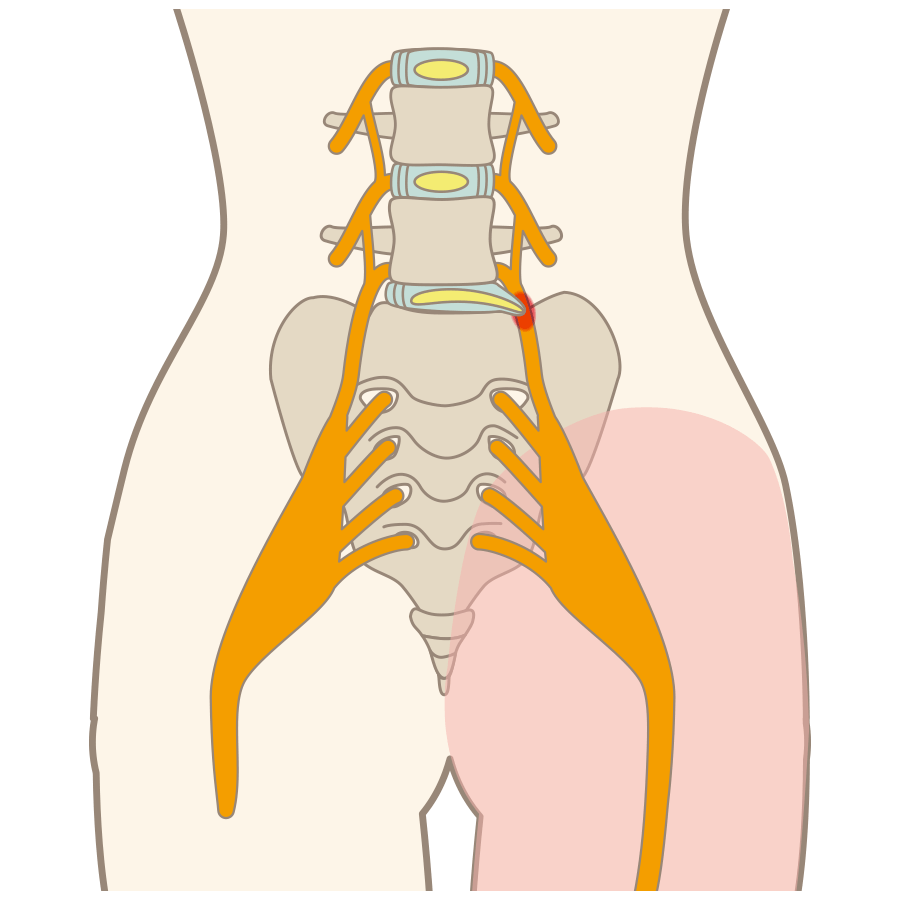
Symptoms such as dullness, sluggishness and heaviness in the lower back and buttocks when you wake up in the morning, when you try to get up from bed, or when you are tired may occur, as well as pain and other symptoms as far as the thighs and calves. You may also experience pain if you remain seated for long periods of time. If the deformity is advanced, neurological symptoms such as intermittent claudication due to spinal stenosis, numbness, paresthesia, or movement disorders may also occur.
Treatments for Lumbar spondylosis of the Lumbar Spine
Conservative treatments
There are two types of treatment: drug therapy and therapeutic exercise.
In some cases, symptoms caused by an impeded blood flow can be relieved by improving the blood circulation, and medication for this purpose may be prescribed. We use therapeutic exercises to prevent aggravation of the stresses caused by the deformity and to correct the lifestyle-induced imbalances in the muscles and joints back into a stress-free state. If no improvement is seen with these methods, surgical treatment may be considered.
Surgical procedures
Surgical procedures are often used to reduce pressure on the nerves, and in the case of spinal stenosis, it involves a procedure called spinal fusion, in which muscles and ligaments are removed in order to secure the unstable bones and, using an endoscope, parts of the lumbar vertebrae and the enlarged ligaments are shaved off in order to suppress the pressure. However, sometimes the inflammation does not go away after the surgery or does not even improve, or the pain may also recur. In this case, factors others than the discs and lumbar spine, such as the physical constitution, muscles, and ligaments, may be involved in the cause of pain, and in this regard, this procedure cannot be considered a root treatment. At our hospital, we recommend a treatment called The Discseel® Procedure, which promotes intervertebral disc repair and regeneration, relieves disc inflammation by stopping its degeneration and also reduce the inflammation from the muscles and ligaments through therapeutic exercise, in combination with therapeutic exercises implemented at the Soma Rehabilitation Center, a rehabilitation facility specialized in low back pain that is affiliated with our clinic.
What treatments offered at our clinic are effective for lumbar spondylosis?
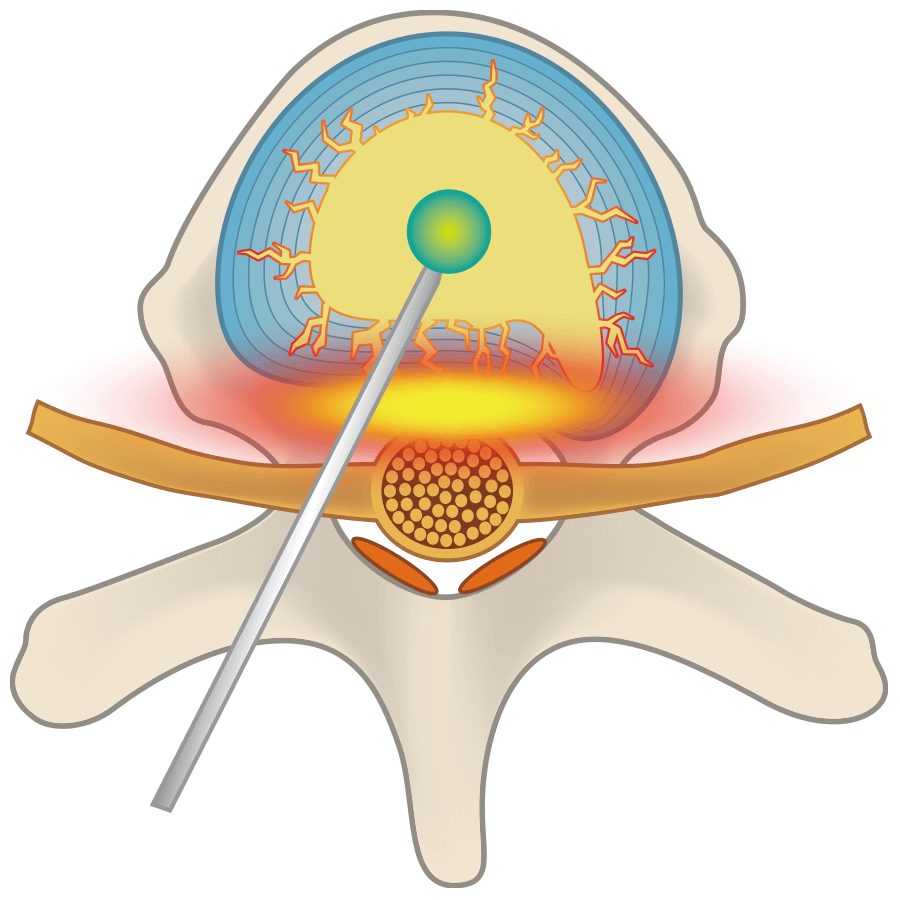
In degenerative lumbar spondylosis, pressure on the nerves and the worsening of symptoms are believed to be caused by a deformed intervertebral disc. Therefore, we believe that if we can suppress the deformation of the intervertebral disc, we can prevent inflammation related to nerve compression, as well as bone deformity and ligament enlargement. In order to achieve this, we perform an intervertebral disc restoration and regeneration treatment using The Discseel® Procedure, which repairs the torn annulus fibrosus and restores intervertebral disc function by replenishing the water content inside the nucleus pulposus. The treatment can be performed as an ambulatory treatment and under local anesthesia in the lower back, with a needle injecting a medical solution into the intervertebral disc. The treatment takes about 25 minutes and is followed by a recovery time of about 1 hour, after which you are allowed to go home.
Treatment Overview
The Discseel
Discseel® Procedure
Discseel® Procedure was developed by an American surgeon by the name of Dr. Kevin Pauza, after caring for hundreds of patients who were made worse following their spine surgery. The treatment aims to seal tears in herniated vertebral discs and help them regenerate and recover their, allowing permanent relief of back pain. Dr. Pauza holds a series of 16 patents for a device and Discseel® biologic that support the treatment. Dr.Nonaka has been licensed to perform the Discseel® Procedure in 2018, and more than 2,880 patient have undergone the treatment in our clinic since then. At present, approximately 20 doctors, including physicians from Harvard and Boston Universities are using the Discseel® Procedure to treat their patients in the USA. Dr. Nonaka is the first physician trained to perform the Discseel® Procedure in Japan.
Lumbar spondylosis: FAQ
-
- Q
-
What are some everyday precautions to take if I have degenerative lumbar spondylosis?
- A
-
If you are diagnosed with degenerative lumbar spondylosis, the first important step is to prevent further degeneration of the disc and bone: reduce the frequency of your movements and tasks, especially if they are strenuous on your lower back, and closely follow your doctor's advice in order to determine the next step.
-
- Q
-
How should I sleep if I have lumbar spondylosis?
- A
-
If you sleep on your back, put a cushion under your knees, and if you sleep on your side, curling up your body will make you feel much relaxed and comfortable.
-
- Q
-
What is the difference between degenerative lumbar spondylosis and a herniated disc?
- A
-
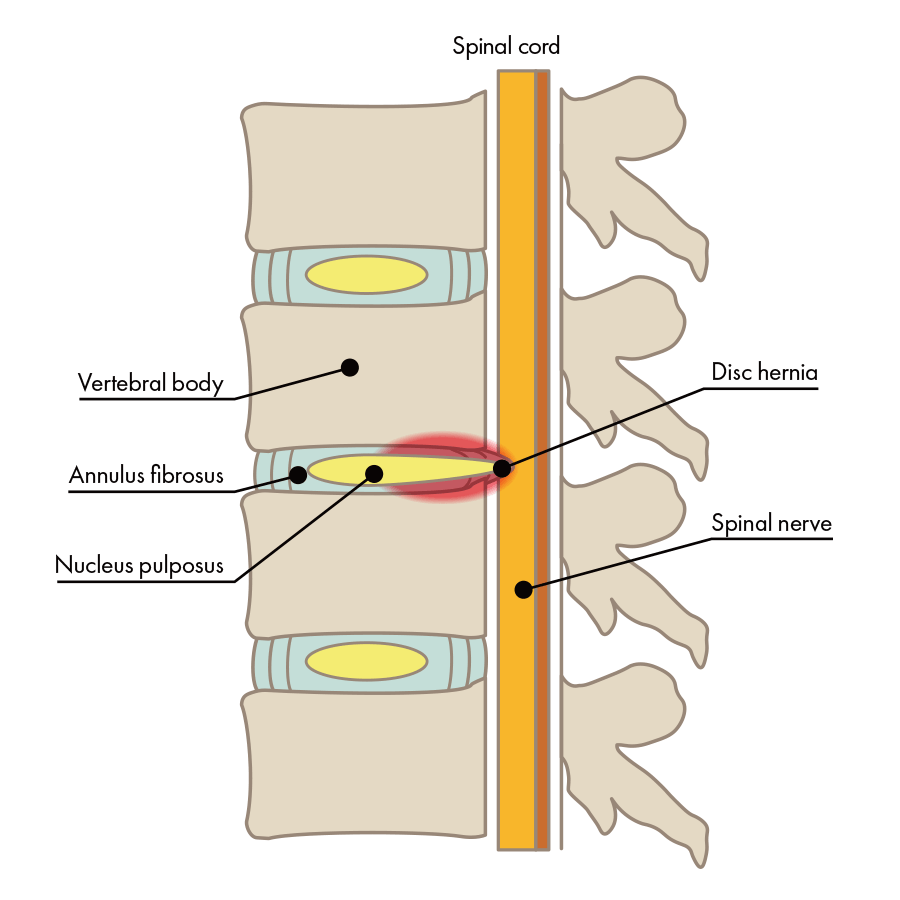
Disc herniation is when the nucleus pulposus inside the disc protrudes and compresses the nerve, causing pain. Degenerative lumbar spondylosis is when pain is caused by degeneration of the disc, enlargement of the ligaments, or the apparition of bone spurs. It may evolve from degenerative lumbar spondylosis to disc herniation or spinal canal stenosis.
-
- Q
-
Can lumbar spondylosis be cured without having recourse to surgery?
- A
-
Unfortunately, if the bone is deformed, it will not cure by itself. By devising a program aimed at improving the patient’s physical constitution, it is possible to reduce inflammation and prevent the aggravation of pain and the progression of symptoms, without having recourse to any treatment tackling the root cause of the problem.
-
- Q
-
Is there any medication that can cure lumbar spondylosis?
- A
-
Medication cannot cure the disease thoroughly as it fails to address the root cause. However, some medications may be prescribed to relieve pain or to improve blood circulation. In case when the pain is severe, painkillers may be administered. Some patients who have been taking prescribed medication for a long time may experience other ailments and side effects if they stop them abruptly, so continuous improvement through therapeutic exercise and treatment while continuing to take the prescription may be privileged.
-
- Q
-
Will I be able to keep on working if I have lumbar spondylosis?
- A
-
Depending on the severity of the symptoms, it may be possible to continue working. However, if your job involves a lot of desk work or heavy labor, it would be preferable to avoid such types of work as it will place extra strain on your back. If you find changing your work environment overnight difficult, consider improving your physical condition, posture, and muscle strength. If these methods improve your quality of life, we recommend pursuing this program. If no improvement is noted, we recommend that you consult a medical facility for a consultation and further diagnosis.
Targeted Conditions
-
Disc Herniation

-
Spinal Canal Stenosis

-
Sciatica

-
Spondylolisthesis

-
Disc Degeneration

-
Lumbar Spondylosis

- HOME/
- Targeted Conditions/
- Lumbar spondylosis